Drug Resistance and Novel Therapies in Cancers
A topical collection in Cancers (ISSN 2072-6694). This collection belongs to the section "Cancer Drug Development".
Viewed by 546402Editor
Interests: receptor tyrosine kinases; EGFR; signal transduction; cancer therapy; breast cancer treatment; targeted therapy
Special Issues, Collections and Topics in MDPI journals
Topical Collection Information
Dear Colleagues,
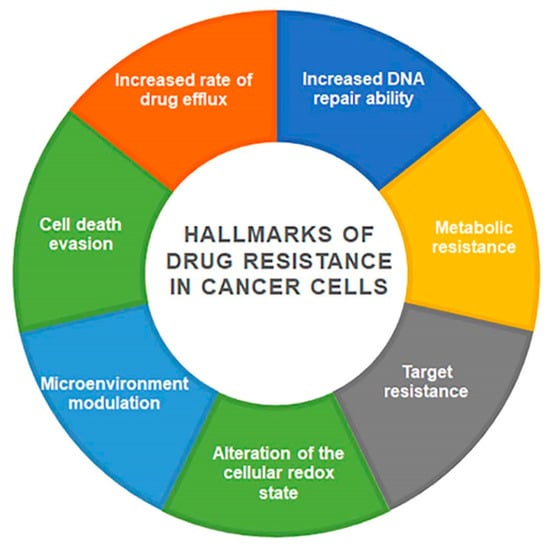
Cancer is among the leading causes of mortality in developed countries. Despite advances in treatment in all settings, disease recurrence and progression remains a major obstacle to therapy. One of the main clinical issues is the development of drug resistance. Drug resistance exists in two forms: Acquired resistance, where the drug is initially efficient but becomes ineffective over time, while intrinsic resistance occurs when a drug is ineffective from the beginning of treatment. The hallmarks of drug resistance in cancers include sustained tumor cell proliferation, insensitive to growth suppressors, resisting cell death, and active invasion.
The early drugs used in cancer treatment are all of chemical origin, and as thus, drug resistance is also called chemoresistance in cancer. However, with the development of novel cancer treatment agents, such as hormones, cytokines, antibodies, antisense oligonucleotides and siRNAs, cancer drugs now could include any agent that is used to treat cancer patients. Therefore the term drug resistance in cancer could be used to cover resistance to any cancer treatment agents.
Through intensive studies, multiple mechanisms have been identified for the development of drug resistance. In general, drug resistance could arise due to decreased intracellular drug concentrations, alterations of drug targets, epigenetic modification, and activation of certain signaling cascades These mechanisms include drug inactivation, drug target alteration, drug efflux, DNA damage repair, cell death inhibition, the epithelial-mesenchymal transition (EMT), and epigenetic modifications.
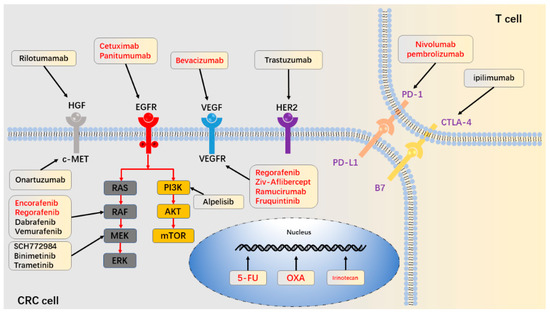
Many strategies have been developed to combat drug resistance, either by combining the currently available therapies or by developing novel therapies. While new chemotherapeutic agents are still developed and chemotherapy is still standard-of-care in the treatment of most cancers, the focus has shift to the development and application of novel therapeutic agents for immunotherapy and targeted therapy due to the improved understanding of tumor biology and the hallmarks of cancers. Targeted therapies have frequently been used in combination with chemotherapeutic agents and radiotherapy in some cases.
Prof. Dr. Zhixiang Wang
Collection Editor
Manuscript Submission Information
Manuscripts should be submitted online at www.mdpi.com by registering and logging in to this website. Once you are registered, click here to go to the submission form. Manuscripts can be submitted until the deadline. All submissions that pass pre-check are peer-reviewed. Accepted papers will be published continuously in the journal (as soon as accepted) and will be listed together on the collection website. Research articles, review articles as well as communications are invited. For planned papers, a title and short abstract (about 100 words) can be sent to the Editorial Office for announcement on this website.
Submitted manuscripts should not have been published previously, nor be under consideration for publication elsewhere (except conference proceedings papers). All manuscripts are thoroughly refereed through a single-blind peer-review process. A guide for authors and other relevant information for submission of manuscripts is available on the Instructions for Authors page. Cancers is an international peer-reviewed open access semimonthly journal published by MDPI.
Please visit the Instructions for Authors page before submitting a manuscript. The Article Processing Charge (APC) for publication in this open access journal is 2900 CHF (Swiss Francs). Submitted papers should be well formatted and use good English. Authors may use MDPI's English editing service prior to publication or during author revisions.
Keywords
- cancer
- chemotherapy
- novel therapy
- drug resistance
- multidrug resistance
- intrinsic drug resistance
- acquired drug resistance
- metastasis
- apoptosis
- disease recurrence
- targeted therapy
- immunotherapy
- hormones
- cytokines
- antibodies
- antisense oligonucleotides
- siRNAs