Innovations in Cancer Drug Development Research
Share This Topical Collection
Editor
Topical Collection Information
Dear Colleagues,
This Topical Collection, titled “Innovations in Cancer Drug Development Research”, will bring together groundbreaking research into cancer drug development. Currently, scientists and researchers are exploring revolutionary approaches to enhance the efficacy of cancer treatments and alleviate side effects experienced by patients. Innovations encompass the discovery of new drug targets, the development of more efficient drug delivery systems, and the utilization of advanced technologies and methods, such as gene editing and artificial intelligence, to expedite the discovery and development of new drugs. Through these innovations, researchers will personalize treatments and both gain a better understanding of and learn how to overcome drug resistance, providing cancer patients with more viable and enduring therapeutic options. Ongoing innovative research in this field continues to advance cancer treatments, offering patients greater hope and improved chances of survival.
Original research papers reporting in vitro and in vivo data; authoritative systematic, and perspective reviews; clinical trials; and reports on meta-analysis will be considered. Various relevant topics include, but are not limited to, the following areas:
- Anticancer drug discovery;
- Drug development;
- Chemotherapeutic agents;
- Hormonal agents;
- Targeted agents;
- Immunological agents;
- Preventive therapeutic agents;
- Radiopharmaceuticals;
- Combination therapies;
- Structure–activity relationship;
- Dereplication and molecular networking;
- Pharmacokinetics of anticancer agents;
- Emerging hallmarks;
- Precision medicine;
- Personalized therapy;
- Artificial intelligence.
Prof. Dr. Anupam Bishayee
Collection Editor
Manuscript Submission Information
Manuscripts should be submitted online at www.mdpi.com by registering and logging in to this website. Once you are registered, click here to go to the submission form. Manuscripts can be submitted until the deadline. All submissions that pass pre-check are peer-reviewed. Accepted papers will be published continuously in the journal (as soon as accepted) and will be listed together on the collection website. Research articles, review articles as well as communications are invited. For planned papers, a title and short abstract (about 100 words) can be sent to the Editorial Office for announcement on this website.
Submitted manuscripts should not have been published previously, nor be under consideration for publication elsewhere (except conference proceedings papers). All manuscripts are thoroughly refereed through a single-blind peer-review process. A guide for authors and other relevant information for submission of manuscripts is available on the Instructions for Authors page. Cancers is an international peer-reviewed open access semimonthly journal published by MDPI.
Please visit the Instructions for Authors page before submitting a manuscript.
The Article Processing Charge (APC) for publication in this open access journal is 2900 CHF (Swiss Francs).
Submitted papers should be well formatted and use good English. Authors may use MDPI's
English editing service prior to publication or during author revisions.
Keywords
- drug resistance
- novel drug formulation
- novel drug delivery
Published Papers (8 papers)
2024
Open AccessReview
Antibody-Drug Conjugates and Their Potential in the Treatment of Patients with Biliary Tract Cancer
by
Shaun Alexander, Umair Aleem, Timothy Jacobs, Melissa Frizziero, Victoria Foy, Richard A. Hubner and Mairéad G. McNamara
Viewed by 1298
Abstract
Background: Biliary tract cancers (BTCs) are aggressive in nature, often presenting asymptomatically until they are diagnosed at an advanced stage. Surgical resection or liver transplantation are potential curative options. However, a large proportion of patients present with incurable locally advanced or metastatic disease
[...] Read more.
Background: Biliary tract cancers (BTCs) are aggressive in nature, often presenting asymptomatically until they are diagnosed at an advanced stage. Surgical resection or liver transplantation are potential curative options. However, a large proportion of patients present with incurable locally advanced or metastatic disease and most of these patients are only eligible for palliative chemotherapy or best supportive care. More recently, targeted therapies have proven beneficial in a molecularly selected subgroup of patients with cholangiocarcinoma who have progressed on previous lines of systemic treatment. However, only a minority of patients with BTCs whose tumours harbour specific molecular alterations can access these therapies.
Methods: In relation to ADCs, studies regarding use of antibody–drug conjugates in cancer, particularly in BTCs, were searched in Embase (1974 to 2024) and Ovid MEDLINE(R) (1946 to 2024) to obtain relevant articles. Examples of current clinical trials utilising ADC treatment in BTCs were extracted from the ClinicalTrials.gov trial registry.
Conclusions: Overall, this review has highlighted that ADCs have shown encouraging outcomes in cancer therapy, and this should lead to further research including in BTCs, where treatment options are often limited. The promising results observed with ADCs in various cancers underscore their potential as a transformative approach in oncology, warranting continued exploration and development and the need for education on the management of their specific toxicities. By addressing current challenges and optimising ADC design and application, future studies could potentially improve treatment outcomes for patients with BTCs and beyond, potentially in both early and advanced stage settings.
Full article
►▼
Show Figures
Open AccessReview
Short Peptides as Powerful Arsenal for Smart Fighting Cancer
by
Joanna Bojarska and Wojciech M. Wolf
Viewed by 1167
Abstract
Short peptides have been coming around as a strong weapon in the fight against cancer on all fronts—in immuno-, chemo-, and radiotherapy, and also in combinatorial approaches. Moreover, short peptides have relevance in cancer imaging or 3D culture. Thanks to the natural ‘smart’
[...] Read more.
Short peptides have been coming around as a strong weapon in the fight against cancer on all fronts—in immuno-, chemo-, and radiotherapy, and also in combinatorial approaches. Moreover, short peptides have relevance in cancer imaging or 3D culture. Thanks to the natural ‘smart’ nature of short peptides, their unique structural features, as well as recent progress in biotechnological and bioinformatics development, short peptides are playing an enormous role in evolving cutting-edge strategies. Self-assembling short peptides may create excellent structures to stimulate cytotoxic immune responses, which is essential for cancer immunotherapy. Short peptides can help establish versatile strategies with high biosafety and effectiveness. Supramolecular short peptide-based cancer vaccines entered clinical trials. Peptide assemblies can be platforms for the delivery of antigens, adjuvants, immune cells, and/or drugs. Short peptides have been unappreciated, especially in the vaccine aspect. Meanwhile, they still hide the undiscovered unlimited potential. Here, we provide a timely update on this highly active and fast-evolving field.
Full article
Open AccessArticle
Treosulfan-Versus Melphalan-Based Reduced Intensity Conditioning in HLA-Haploidentical Transplantation for Patients ≥ 50 Years with Advanced MDS/AML
by
Alessia Fraccaroli, Elena Stauffer, Sarah Haebe, Dusan Prevalsek, Lena Weiss, Klara Dorman, Heidrun Drolle, Michael von Bergwelt-Baildon, Hans-Joachim Stemmler, Tobias Herold and Johanna Tischer
Viewed by 1031
Abstract
Relapse and regimen-related toxicities remain major challenges in achieving long-term survival, particularly among older patients with high-risk myelodysplastic syndrome (MDS) or acute myeloid leukemia (AML) undergoing allogeneic hematopoietic stem cell transplantation (allo-HSCT). Previous studies have demonstrated the feasibility of treosulfan-based conditioning, noting stable
[...] Read more.
Relapse and regimen-related toxicities remain major challenges in achieving long-term survival, particularly among older patients with high-risk myelodysplastic syndrome (MDS) or acute myeloid leukemia (AML) undergoing allogeneic hematopoietic stem cell transplantation (allo-HSCT). Previous studies have demonstrated the feasibility of treosulfan-based conditioning, noting stable engraftment and low non-relapse mortality (NRM) in patients undergoing HLA-matched allo-HSCT. However, data on treosulfan-based conditioning in the HLA-haploidentical transplantation (HaploT) setting are limited. We retrospectively compared conditioning with fludarabine–cyclophosphamide (FC)–melphalan (110 mg/m
2) and FC-treosulfan (30 g/m
2) prior to HaploT using post-transplantation cyclophosphamide (PTCy) in patients with high-risk MDS/AML patients ≥ 50 years, transplanted from 2009–2021 at our institution (
n = 80). After balancing patient characteristics by a matched-pair analysis, we identified twenty-one matched pairs. Two-year OS and LFS were similar among the groups (OS 66% and LFS 66%,
p = 0.8 and
p = 0.57). However, FC-melphalan was associated with a significantly lower probability of relapse compared to FC-treosulfan (0% vs. 24%,
p = 0.006), counterbalanced by a higher NRM (33% vs. 10%,
p = 0.05). Time to engraftment and incidences of acute and chronic graft-versus-host disease (GvHD) did not differ significantly. In conclusion, HaploT using FC-treosulfan in combination with PTCy in patients aged ≥50 years with MDS/AML appears safe and effective, particularly in advanced disease stages. We confirm the favorable extramedullary toxicity profile, allowing for potential dose intensification to enhance antileukemic activity.
Full article
►▼
Show Figures
Open AccessArticle
Anticancer Effect of PtIIPHENSS, PtII5MESS, PtII56MESS and Their Platinum(IV)-Dihydroxy Derivatives against Triple-Negative Breast Cancer and Cisplatin-Resistant Colorectal Cancer
by
Maria George Elias, Shadma Fatima, Timothy J. Mann, Shawan Karan, Meena Mikhael, Paul de Souza, Christopher P. Gordon, Kieran F. Scott and Janice R. Aldrich-Wright
Cited by 1 | Viewed by 1467
Abstract
Development of resistance to cisplatin, oxaliplatin and carboplatin remains a challenge for their use as chemotherapies, particularly in breast and colorectal cancer. Here, we compare the anticancer effect of novel complexes [Pt(1,10-phenanthroline)(1
S,2
S-diaminocyclohexane)](NO
3)
2 (
PtIIPHEN
[...] Read more.
Development of resistance to cisplatin, oxaliplatin and carboplatin remains a challenge for their use as chemotherapies, particularly in breast and colorectal cancer. Here, we compare the anticancer effect of novel complexes [Pt(1,10-phenanthroline)(1
S,2
S-diaminocyclohexane)](NO
3)
2 (
PtIIPHENSS), [Pt(5-methyl-1,10-phenanthroline)(1
S,2
S-diaminocyclohexane)](NO
3)
2 (
PtII5MESS) and [Pt(5,6-dimethyl-1,10-phenanthroline)(1
S,2
S-diaminocyclohexane)](NO
3)
2 (
PtII56MESS) and their platinum(IV)-dihydroxy derivatives with cisplatin. Complexes are greater than 11-fold more potent than cisplatin in both 2D and 3D cell line cultures with increased selectivity for cancer cells over genetically stable cells. ICP-MS studies showed cellular uptake occurred through an active transport mechanism with considerably altered platinum concentrations found in the cytoskeleton across all complexes after 24 h. Significant reactive oxygen species generation was observed, with reduced mitochondrial membrane potential at 72 h of treatment. Late apoptosis/necrosis was shown by Annexin V-FITC/PI flow cytometry assay, accompanied by increased sub-G0/G1 cells compared with untreated cells. An increase in S and G2+M cells was seen with all complexes. Treatment resulted in significant changes in actin and tubulin staining. Intrinsic and extrinsic apoptosis markers, MAPK/ERK and PI3K/AKT activation markers, together with autophagy markers showed significant activation of these pathways by Western blot. The proteomic profile investigated post-72 h of treatment identified 1597 MDA−MB−231 and 1859 HT29 proteins quantified by mass spectroscopy, with several differentially expressed proteins relative to no treatment. GO enrichment analysis revealed a statistically significant enrichment of RNA/DNA-associated proteins in both the cell lines and specific additional processes for individual drugs. This study shows that these novel agents function as multi-mechanistic chemotherapeutics, offering promising anticancer potential, and thereby supporting further research into their application as cancer therapeutics.
Full article
►▼
Show Figures
Open AccessReview
Overcoming Chemoresistance in Cancer: The Promise of Crizotinib
by
Sanaa Musa, Noor Amara, Adan Selawi, Junbiao Wang, Cristina Marchini, Abed Agbarya and Jamal Mahajna
Cited by 2 | Viewed by 2358
Abstract
Chemoresistance is a major obstacle in cancer treatment, often leading to disease progression and poor outcomes. It arises through various mechanisms such as genetic mutations, drug efflux pumps, enhanced DNA repair, and changes in the tumor microenvironment. These processes allow cancer cells to
[...] Read more.
Chemoresistance is a major obstacle in cancer treatment, often leading to disease progression and poor outcomes. It arises through various mechanisms such as genetic mutations, drug efflux pumps, enhanced DNA repair, and changes in the tumor microenvironment. These processes allow cancer cells to survive despite chemotherapy, underscoring the need for new strategies to overcome resistance and improve treatment efficacy. Crizotinib, a first-generation multi-target kinase inhibitor, is approved by the FDA for the treatment of ALK-positive or ROS1-positive non-small cell lung cancer (NSCLC), refractory inflammatory (ALK)-positive myofibroblastic tumors (IMTs) and relapsed/refractory ALK-positive anaplastic large cell lymphoma (ALCL). Crizotinib exists in two enantiomeric forms: (R)-crizotinib and its mirror image, (S)-crizotinib. It is assumed that the R-isomer is responsible for the carrying out various processes reviewed here The S-isomer, on the other hand, shows a strong inhibition of MTH1, an enzyme important for DNA repair mechanisms. Studies have shown that crizotinib is an effective multi-kinase inhibitor targeting various kinases such as c-Met, native/T315I Bcr/Abl, and JAK2. Its mechanism of action involves the competitive inhibition of ATP binding and allosteric inhibition, particularly at Bcr/Abl. Crizotinib showed synergistic effects when combined with the poly ADP ribose polymerase inhibitor (PARP), especially in ovarian cancer harboring BRCA gene mutations. In addition, crizotinib targets a critical vulnerability in many p53-mutated cancers. Unlike its wild-type counterpart, the p53 mutant promotes cancer cell survival. Crizotinib can cause the degradation of the p53 mutant, sensitizing these cancer cells to DNA-damaging substances and triggering apoptosis. Interestingly, other reports demonstrated that crizotinib exhibits anti-bacterial activity, targeting Gram-positive bacteria. Also, it is active against drug-resistant strains. In summary, crizotinib exerts anti-tumor effects through several mechanisms, including the inhibition of kinases and the restoration of drug sensitivity. The potential of crizotinib in combination therapies is emphasized, particularly in cancers with a high prevalence of the p53 mutant, such as triple-negative breast cancer (TNBC) and high-grade serous ovarian cancer (HGSOC).
Full article
►▼
Show Figures
Open AccessArticle
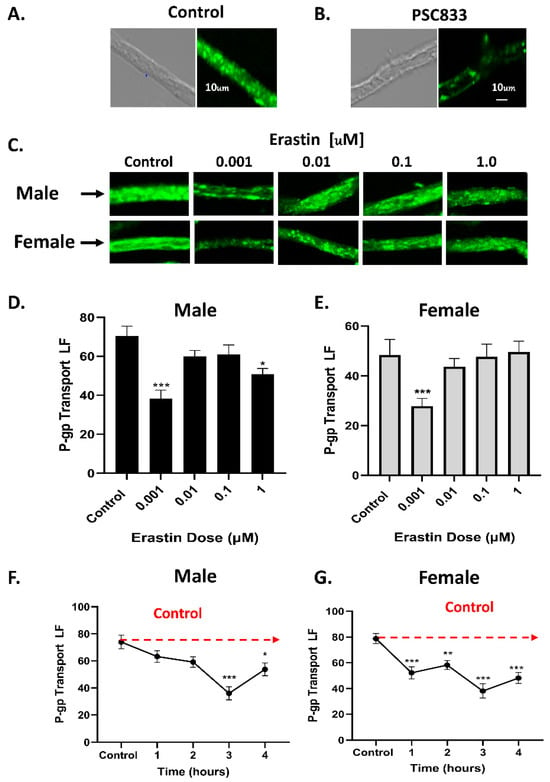
A Role for iNOS in Erastin Mediated Reduction of P-Glycoprotein Transport Activity
by
Shalyn M. Brown, Birandra K. Sinha and Ronald E. Cannon
Cited by 1 | Viewed by 1078
Abstract
The blood–brain barrier is composed of both a physical barrier and an enzymatic barrier. Tight junction (TJ) proteins expressed between endothelial cells of brain capillaries provide the physical barrier to paracellular movement of ions and molecules to the brain, while luminal-facing efflux transporters
[...] Read more.
The blood–brain barrier is composed of both a physical barrier and an enzymatic barrier. Tight junction (TJ) proteins expressed between endothelial cells of brain capillaries provide the physical barrier to paracellular movement of ions and molecules to the brain, while luminal-facing efflux transporters enzymatically restrict the entry of blood-borne molecules from entering the brain. The expression and activity of ATP Binding Cassette transporters or “ABC” transporters in endothelial cells of the BBB and in human tumor cells are dynamically regulated by numerous signaling pathways. P-glycoprotein (P-gp), (ABCB1), is arguably the most studied transporter of the BBB, and in human cell lines. P-glycoprotein transport activity is rapidly inhibited by signaling pathways that call for the rapid production of nitric oxide (NO) from the inducible nitric oxide synthase enzyme, iNOS. This study investigated how nano-molar levels of the selective chemotherapeutic erastin affect the activity or expression of P-glycoprotein transporter in brain capillaries and in human tumor cell lines. We chose erastin because it signals to iNOS for NO production at low concentrations. Furthermore, erastin inhibits the cellular uptake of cystine through the X
C− cystine/glutamate antiporter. Since previous reports indicate that NO production from iNOS can rapidly inhibit P-gp activity in tumor cells, we wondered if induction of iNOS by erastin could also rapidly reduce P-glycoprotein transport activity in brain endothelial cells and in human tumor cell lines. We show here that low concentrations of erastin (1 nM) can induce iNOS, inhibit the activity of P-glycoprotein, and reduce the intracellular uptake of cystine via the Xc- cystine/glutamate antiporter. Consistent with reduced P-glycoprotein activity in rat brain capillary endothelial cells, we show that human tumor cell lines exposed to erastin become more sensitive to cytotoxic substrates of P-glycoprotein.
Full article
►▼
Show Figures
Open AccessReview
Survivin as a Therapeutic Target for the Treatment of Human Cancer
by
Qiang Wang and Mark I. Greene
Viewed by 2110
Abstract
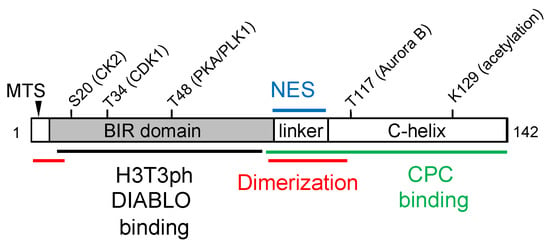
Survivin was initially identified as a member of the inhibitor apoptosis (IAP) protein family and has been shown to play a critical role in the regulation of apoptosis. More recent studies showed that survivin is a component of the chromosome passenger complex and
[...] Read more.
Survivin was initially identified as a member of the inhibitor apoptosis (IAP) protein family and has been shown to play a critical role in the regulation of apoptosis. More recent studies showed that survivin is a component of the chromosome passenger complex and acts as an essential mediator of mitotic progression. Other potential functions of survivin, such as mitochondrial function and autophagy, have also been proposed. Survivin has emerged as an attractive target for cancer therapy because its overexpression has been found in most human cancers and is frequently associated with chemotherapy resistance, recurrence, and poor survival rates in cancer patients. In this review, we discuss our current understanding of how survivin mediates various aspects of malignant transformation and drug resistance, as well as the efforts that have been made to develop therapeutics targeting survivin for the treatment of cancer.
Full article
►▼
Show Figures
Open AccessReview
Targeted Nanoparticle-Based Diagnostic and Treatment Options for Pancreatic Cancer
by
Xin Gu and Tamara Minko
Cited by 7 | Viewed by 3108
Abstract
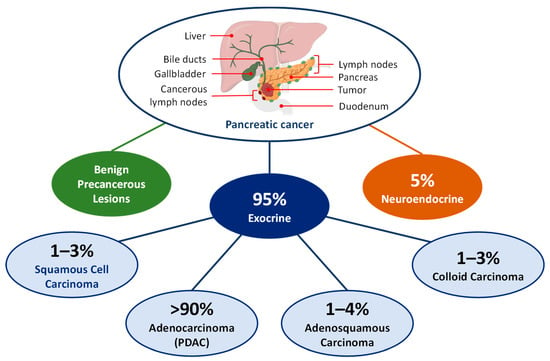
Pancreatic ductal adenocarcinoma (PDAC), one of the deadliest cancers, presents significant challenges in diagnosis and treatment due to its aggressive, metastatic nature and lack of early detection methods. A key obstacle in PDAC treatment is the highly complex tumor environment characterized by dense
[...] Read more.
Pancreatic ductal adenocarcinoma (PDAC), one of the deadliest cancers, presents significant challenges in diagnosis and treatment due to its aggressive, metastatic nature and lack of early detection methods. A key obstacle in PDAC treatment is the highly complex tumor environment characterized by dense stroma surrounding the tumor, which hinders effective drug delivery. Nanotechnology can offer innovative solutions to these challenges, particularly in creating novel drug delivery systems for existing anticancer drugs for PDAC, such as gemcitabine and paclitaxel. By using customization methods such as incorporating conjugated targeting ligands, tumor-penetrating peptides, and therapeutic nucleic acids, these nanoparticle-based systems enhance drug solubility, extend circulation time, improve tumor targeting, and control drug release, thereby minimizing side effects and toxicity in healthy tissues. Moreover, nanoparticles have also shown potential in precise diagnostic methods for PDAC. This literature review will delve into targeted mechanisms, pathways, and approaches in treating pancreatic cancer. Additional emphasis is placed on the study of nanoparticle-based delivery systems, with a brief mention of those in clinical trials. Overall, the overview illustrates the significant advances in nanomedicine, underscoring its role in transcending the constraints of conventional PDAC therapies and diagnostics.
Full article
►▼
Show Figures