The Utility of Biomarkers in Disease Management Approach
A topical collection in Medicina (ISSN 1648-9144). This collection belongs to the section "Translational Medicine".
Viewed by 29890Editors
Interests: acute cardiovascular disease; biomarkers in critical care; sepsis; acute kidney injury
Topical Collection Information
Dear Colleagues,
Traditionally, in a product’s lifecycle, we consider a truth-seeking early stage focused on evaluating novel products’ prospects and eliminating bad bets, and a success-seeking late stage focused on maximizing the value of products that have been cleared for development. However, a third step which is strictly related to the first two is the understanding of the need for innovation, evaluation in the context of the healthcare system, as well as individual patients, and programs to assure that value, not just novelty, supports medical innovation.
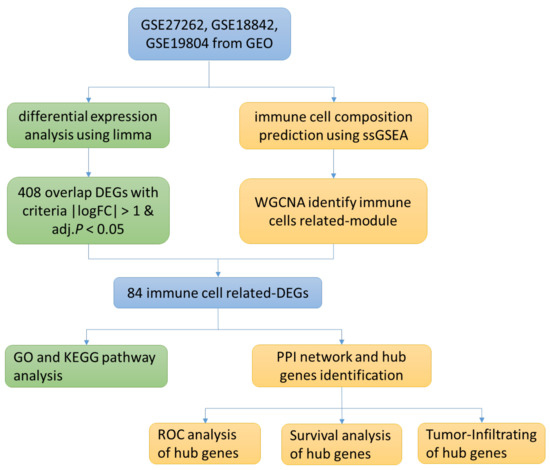
So-called translational research has the ultimate objective of impacting longer-term outcomes with reduced healthcare utilization. One of the most important assumptions at the basis of translational research is that established medical tools can be “optimized” using genetic, biological, and phenotypic information. The scheme below illustrates the steps characterizing translational research:
The unique opportunity to use biomarkers as model for translational medicine:
Researchers navigate the ocean of biomarkers searching for proper targets and their optimal utilization. Emergency medicine builds up the frontline to maximize the utility of clinically validated biomarkers and is the cutting-edge field to test the applicability of promising biomarkers emerging from thorough translational research. The role of biomarkers in clinical decision making would be of greater significance for the identification, risk stratification, monitoring, and prognostication of patients in critical and acute care settings. There is no doubt that basic research to explore novel biomarkers in relation to pathogenesis is as important as its clinical counterpart.
The challenges being faced at the moment include:
- Previously unknown biomarkers;
- Known biomarkers which have either has not been determined routinely or have been determined routinely but not been used for identifying responders for medicine “X”;
- Patient groups of responders which are different to the formerly treated groups;
- Patient groups of responders which overlap a) substantially or b) not substantially with the formerly treated groups;
- Patient groups of responders which are a) smaller or b) bigger subgroups of the formerly treated groups.
You are kindly invited to submit your manuscript on “The Utility of Biomarkers in Disease Management Approach” for a Special Issue of Medicina.
Prof. Dr. Salvatore Di Somma
Dr. David Brenner
Guest Editors
Manuscript Submission Information
Manuscripts should be submitted online at www.mdpi.com by registering and logging in to this website. Once you are registered, click here to go to the submission form. Manuscripts can be submitted until the deadline. All submissions that pass pre-check are peer-reviewed. Accepted papers will be published continuously in the journal (as soon as accepted) and will be listed together on the collection website. Research articles, review articles as well as short communications are invited. For planned papers, a title and short abstract (about 100 words) can be sent to the Editorial Office for announcement on this website.
Submitted manuscripts should not have been published previously, nor be under consideration for publication elsewhere (except conference proceedings papers). All manuscripts are thoroughly refereed through a single-blind peer-review process. A guide for authors and other relevant information for submission of manuscripts is available on the Instructions for Authors page. Medicina is an international peer-reviewed open access monthly journal published by MDPI.
Please visit the Instructions for Authors page before submitting a manuscript. The Article Processing Charge (APC) for publication in this open access journal is 2200 CHF (Swiss Francs). Submitted papers should be well formatted and use good English. Authors may use MDPI's English editing service prior to publication or during author revisions.
Keywords
- translational medicine
- biomarkers
- biomarkers in acute diseases
- biomarkers in chronic disease monitoring
- biomarkers and therapeutic decision making