Advances in Musculoskeletal Tissue Regeneration Using Mesenchymal Stromal/Stem Cells, Biomaterials, and Signaling Molecules
A special issue of Cells (ISSN 2073-4409). This special issue belongs to the section "Stem Cells".
Deadline for manuscript submissions: closed (31 January 2024) | Viewed by 16386
Special Issue Editors
Interests: mesenchymal stem cells/multipotential stromal cells (MSCs); MSC trophic and immunomodulatory actions; MSC functionalization ex vivo; inflammation and fibrosis reversal; synovitis; osteoarthritis; regenerative sports medicine; regenerative orthopaedics
Special Issues, Collections and Topics in MDPI journals
Interests: stem cell research; biomedical engineering; kinesiology; osteoarthritis; regenerative sports medicine; regenerative orthopaedics
Special Issues, Collections and Topics in MDPI journals
Special Issue Information
Dear Colleagues,
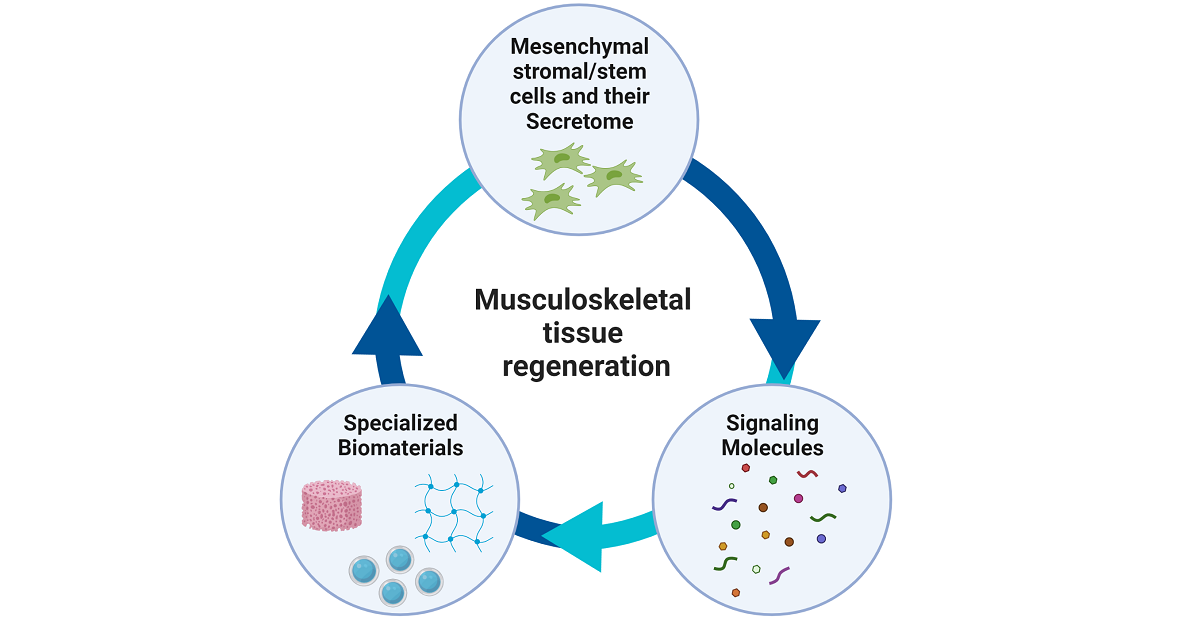
Regeneration of musculoskeletal tissues is a serious clinical challenge given that their injury and disease are leading causes of physical disability worldwide. Approved mesenchymal stromal/stem cells (MSC) and MSC products (i.e., extracellular vesicles) for stem cell-based therapy applications offer huge promise to rejuvenate musculoskeletal tissues, triggering tissue repair and healing. In parallel, the discovery of specialized biomaterials and signaling molecules has opened novel therapeutic avenues as part of tissue engineering approaches. Up-to-date, significant progress has been made in developing and optimizing the components of this therapeutic triad (cells, biomaterials, signaling molecules), but only a limited number of technologies have been successfully transferred into the clinical setting. Currently, efforts are focused on bringing closer basic science and cell-based product manufacturing techniques to potential clinical protocols. This Special Issue aims to present a state-of-the-art update on the use of MSC, biomaterials and signaling molecules for musculoskeletal therapeutic applications.
We are pleased to invite you as a recognized expert in the field to contribute original articles, communications, and reviews covering the entire field of musculoskeletal regeneration research, including (but not limited to):
- MSC and biomaterial functionalization (e.g., cell phenotype-based purification, cell priming, gene-activated matrices);
- MSC-derived extracellular vesicle isolation and methods to reinforce their therapeutic signatures;
- Benefits and limitations of MSC versus MSC-derived extracellular vesicles for musculoskeletal applications;
- MSC and MSC-derived extracellular vesicle effects on immunomodulation and senescent cell clearance;
- Potent signaling molecules to promote healing, reduce inflammation, and stimulate cellular communication;
- Novel specialized biomaterials and scaffolds utilized to regenerate musculoskeletal tissues;
- Microphysiological systems (organ or tissue chips), are generated according to musculoskeletal tissue engineering principles, as drug testing models.
We look forward to hearing any questions you may have and hopefully receiving your contributions.
Dr. Dimitrios Kouroupis
Dr. Thomas M. Best
Guest Editors
Manuscript Submission Information
Manuscripts should be submitted online at www.mdpi.com by registering and logging in to this website. Once you are registered, click here to go to the submission form. Manuscripts can be submitted until the deadline. All submissions that pass pre-check are peer-reviewed. Accepted papers will be published continuously in the journal (as soon as accepted) and will be listed together on the special issue website. Research articles, review articles as well as short communications are invited. For planned papers, a title and short abstract (about 100 words) can be sent to the Editorial Office for announcement on this website.
Submitted manuscripts should not have been published previously, nor be under consideration for publication elsewhere (except conference proceedings papers). All manuscripts are thoroughly refereed through a single-blind peer-review process. A guide for authors and other relevant information for submission of manuscripts is available on the Instructions for Authors page. Cells is an international peer-reviewed open access semimonthly journal published by MDPI.
Please visit the Instructions for Authors page before submitting a manuscript. The Article Processing Charge (APC) for publication in this open access journal is 2700 CHF (Swiss Francs). Submitted papers should be well formatted and use good English. Authors may use MDPI's English editing service prior to publication or during author revisions.
Keywords
- mesenchymal stromal/stem cells
- extracellular vesicles
- biomaterials
- signaling molecules
- microphysiological systems
- musculoskeletal regeneration
- immunomodulation
- cell therapy
- tissue engineering
Benefits of Publishing in a Special Issue
- Ease of navigation: Grouping papers by topic helps scholars navigate broad scope journals more efficiently.
- Greater discoverability: Special Issues support the reach and impact of scientific research. Articles in Special Issues are more discoverable and cited more frequently.
- Expansion of research network: Special Issues facilitate connections among authors, fostering scientific collaborations.
- External promotion: Articles in Special Issues are often promoted through the journal's social media, increasing their visibility.
- e-Book format: Special Issues with more than 10 articles can be published as dedicated e-books, ensuring wide and rapid dissemination.
Further information on MDPI's Special Issue polices can be found here.







